Common Causes of Infertility
What is infertility?
Infertility is generally defined as the inability to achieve conception despite one year of frequent unprotected intercourse. However, there are many instances in which it is reasonable for the male and female to be evaluated sooner than one year.
There can be several reasons why a couple cannot conceive a pregnancy. 1/3 is due to a male factor, 1/3 is due to a female factor and 1/3 is due to couple issues. Therefore 2/3’s of the problem can be rectified if the male issue is identified. The typical male infertility work up is started with a history and physical followed by a semen analysis. If the semen analysis is normal the work up is complete. If it is abnormal, then additional testing is required.
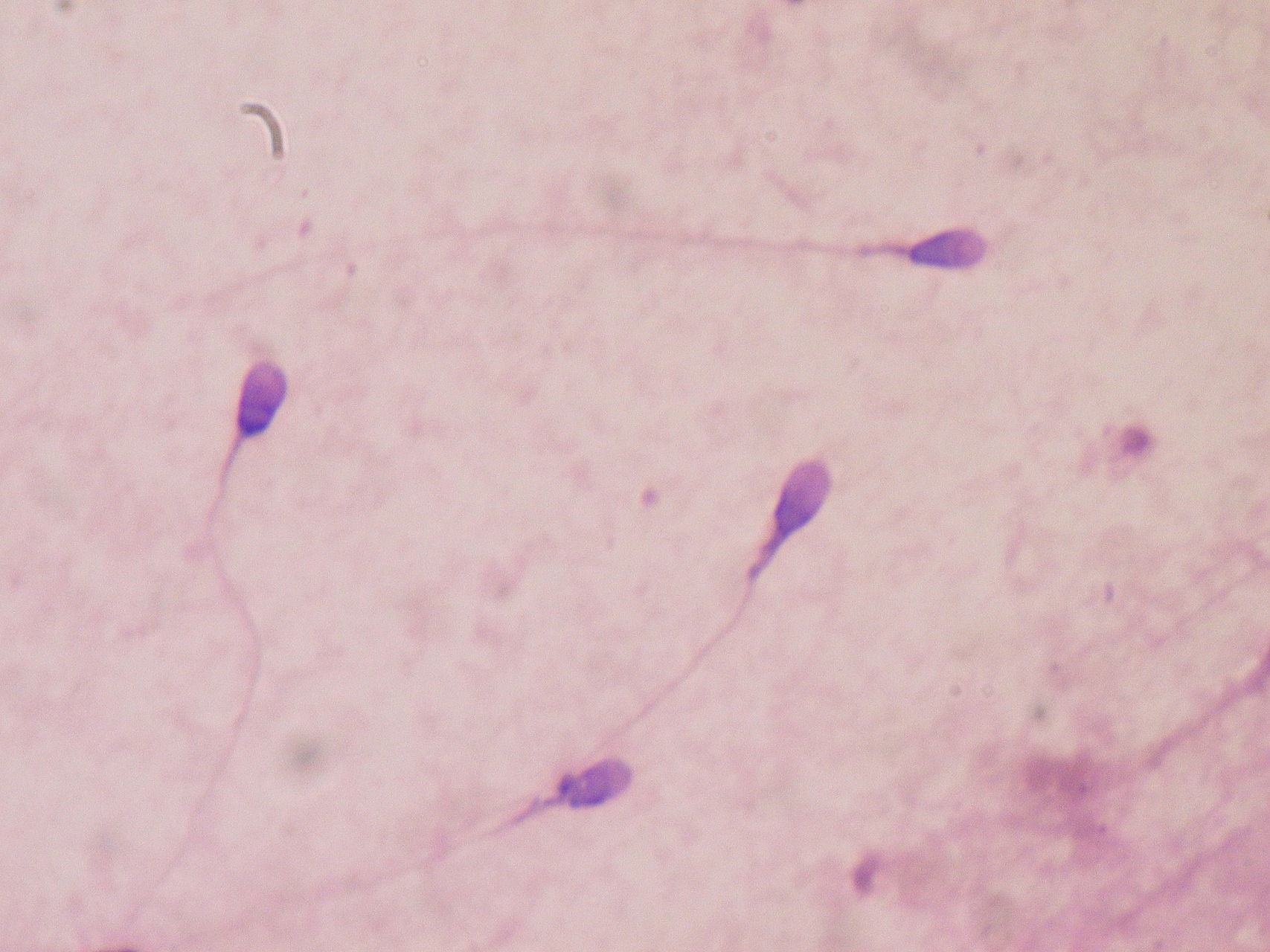
What causes infertility?
Common issues that can be identified are:
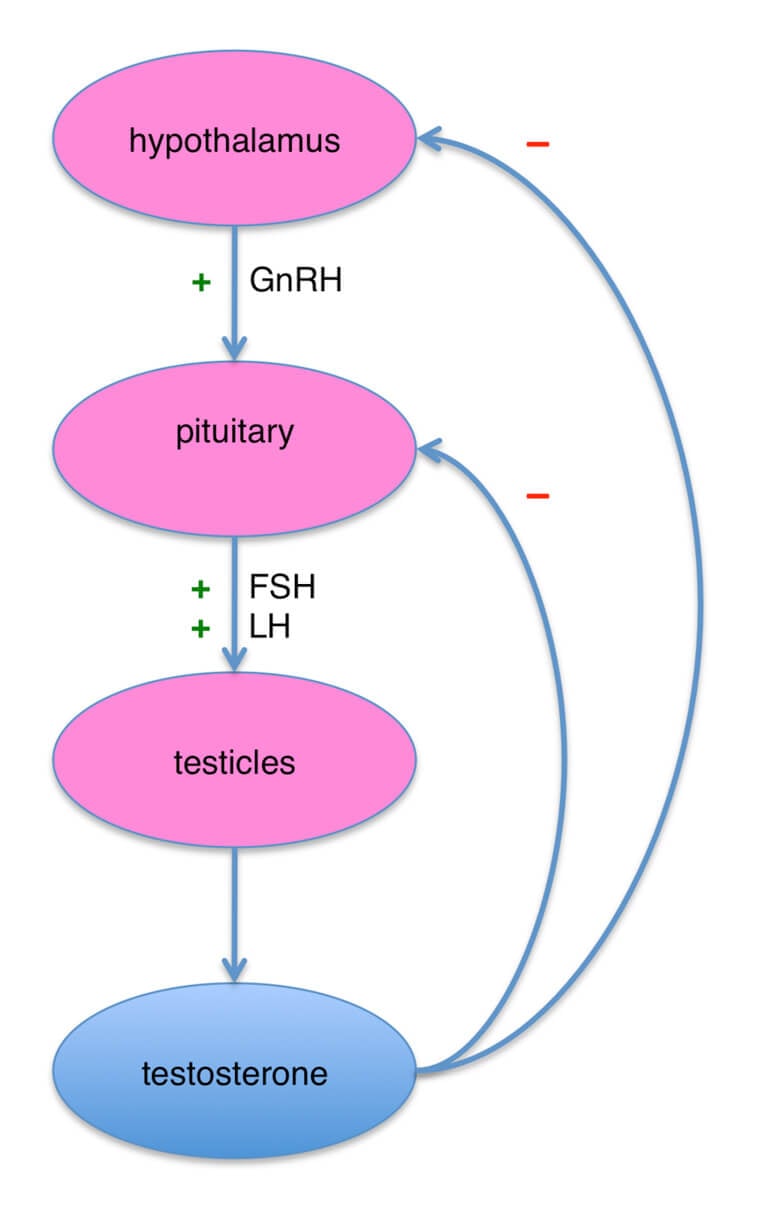
Hormone Imbalance - for a variety of reasons, a man testosterone level may be low, or there may be an imbalance between the male hormone (testosterone) and female hormone (estrogen). There are medications which may be used to help bring this imbalance back into a more normal range which may improve fertility.
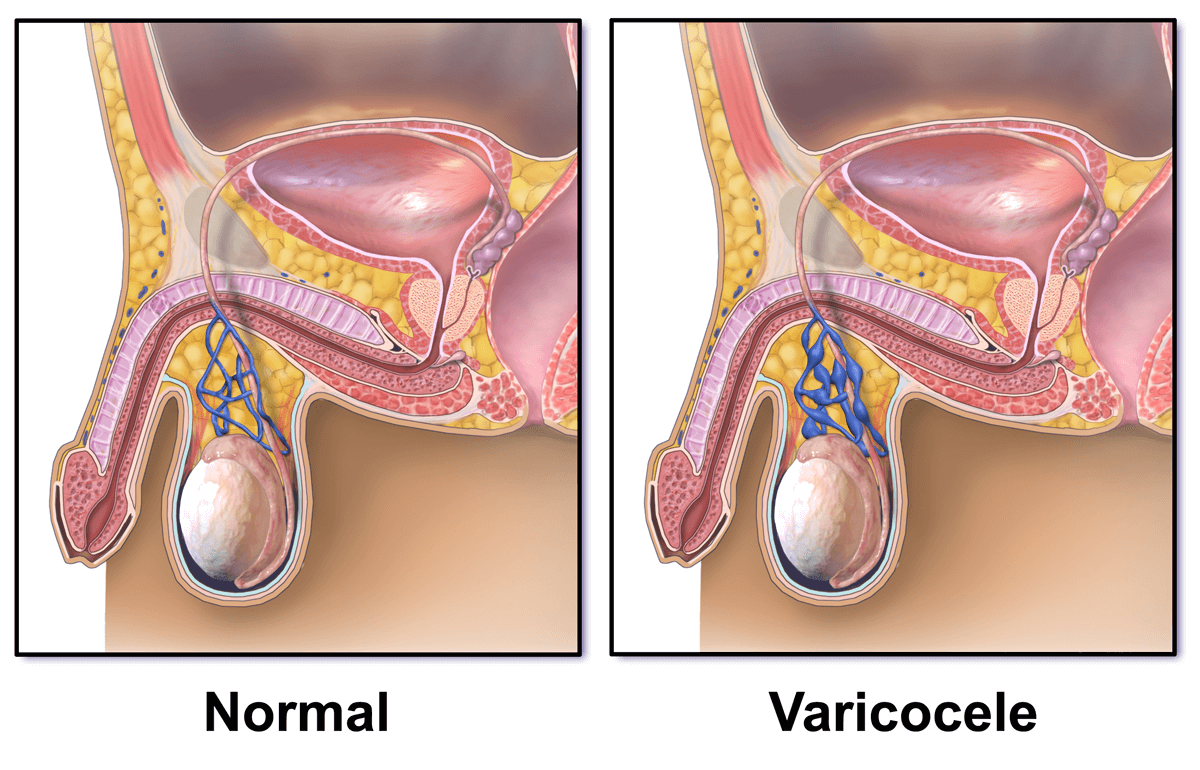
Varicocele – A varicocele is a dilation of a vein (a varicose vein) in the scrotum. Many men with varicoceles have a low sperm count or abnormal sperm morphology (shape). The reason a varicocele affects the sperm may be related to a higher-than-normal temperature in the testicles. Varicocele can be treated with an outpatient surgical procedure.
Exogenous Testosterone Administration - We are finding men of reproductive ages are being placed on testosterone replacement. Almost invariably this will drive sperm count to zero, and may takes months to return.
Poorly timed intercourse – sometimes the timing of intercourse is not in sync with ovulation. Medications that cause poor sperm parameters – once they are stopped the sperm parameters normalize.
More complex problems include obstructive and non-obstructive azoospermia (no sperm in the ejaculate). The diagnosis is made with a semen analysis and a testicular biopsy. There is no treatment for non- obstructive azoospermia.
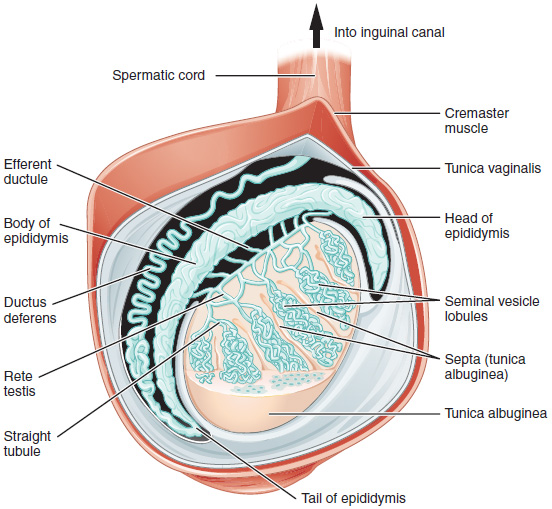
What are next steps?
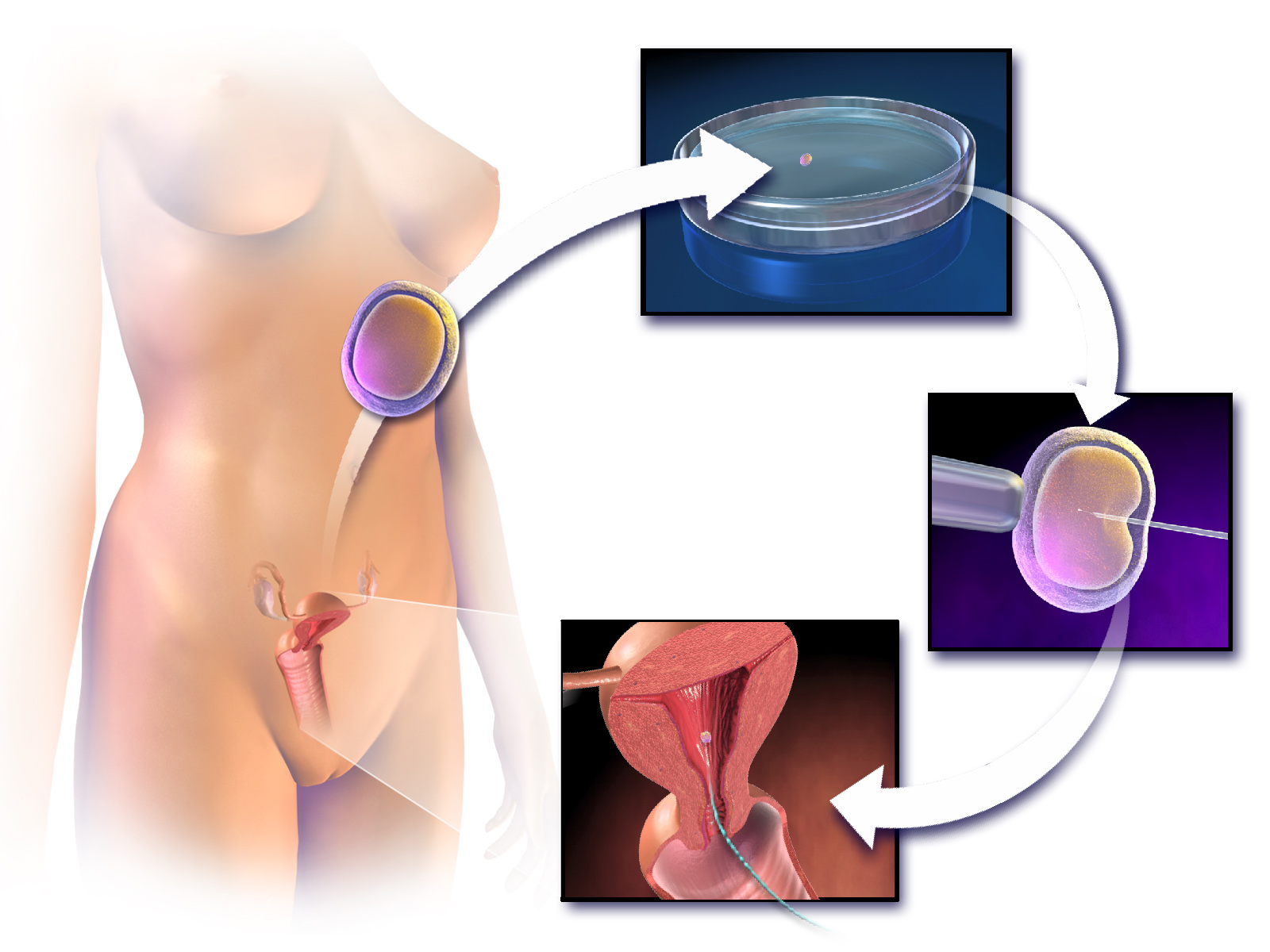
If a patient has normal testicular size, normal serum FSH, LH and testosterone levels and azoospermia, the likely diagnosis is obstructive azoospermia. Obstructive azoospermia is treated with a testicular sperm aspiration (removal of sperm from the testes). This is done by Testicular Biopsy or by using a fine needle to aspirate sperm under anesthesia. The female patient then undergoes an IVF induction and once the eggs are extracted, the sperm are injected, microscopically into the eggs to achieve fertilization. This process is known as Intracytoplasmic Sperm Injection (ICSI). ICSI has revolutionized the treatment and improved the prognosis of male infertility.
Contact us to request an appointment or ask a question. We're here for you.



